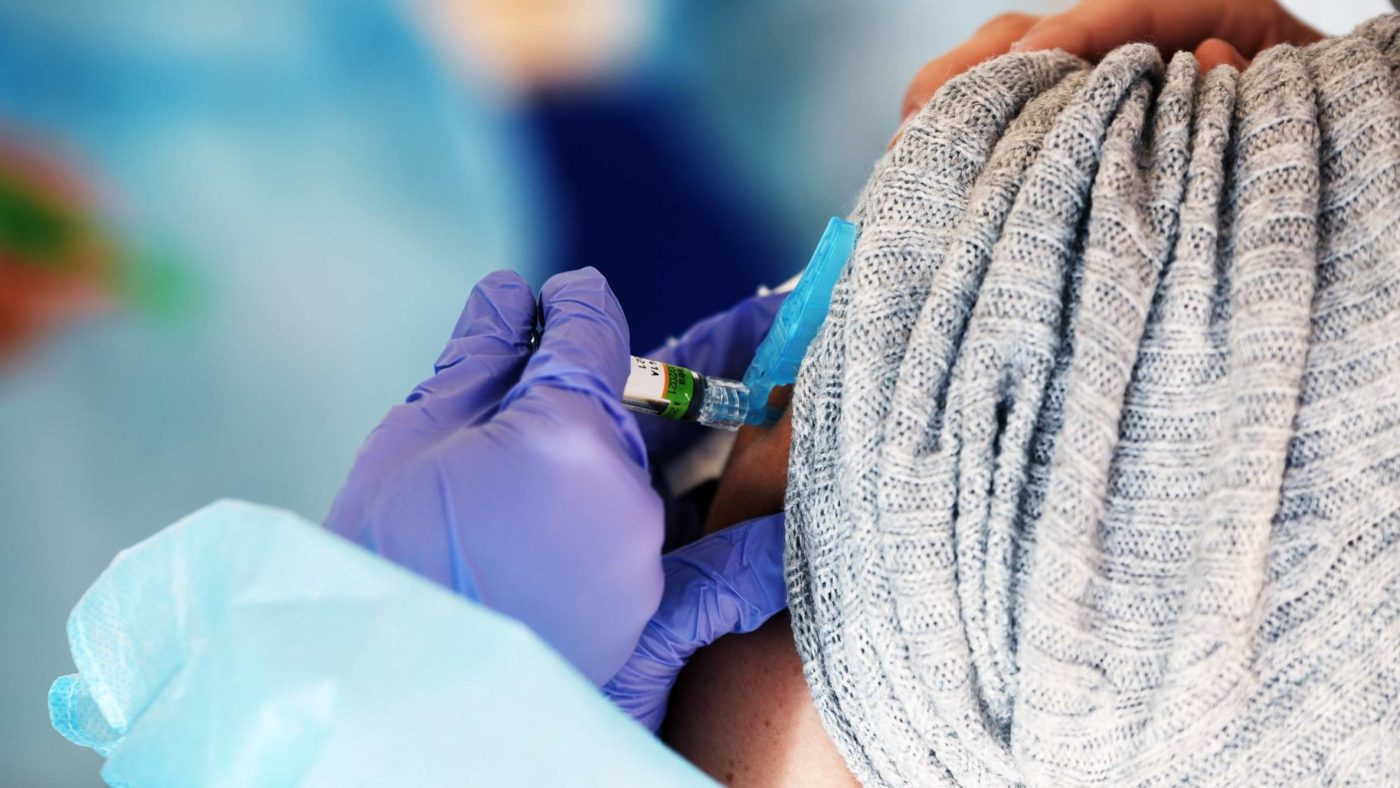
There are currently 11 Covid-19 vaccines in late-stage trials and over 200 others being developed.
When one is finally approved as safe and effective, the next challenge will be persuading enough people to get immunised. But many may be reluctant to do so, thanks to a combination of caution given the unprecedented speed of vaccine development, pseudoscientific scaremongering, and the belief that young people need not bother, given their relatively low Covid mortality risk.
That creates a problem for all of us, since vaccines are rarely 100% effective. To achieve sustainable herd immunity, and protect those who either cannot be vaccinated or whose vaccinations are ineffective, we will need almost everyone who can get vaccinated safely to do so.
The answer may be to pay people to do it, and let the incentive of cold, hard cash take on whatever doubts or reluctance people may have.
The Government has used payments to incentivise people already during the pandemic. Eat Out to Help Out successfully enticed punters into restaurants by part-paying people’s bills. The rationale was that people going to restaurants would show it was ‘business as usual’, bringing social benefits above and beyond the benefit to the diner of a subsidised meal (unfortunately, this appears to have helped spread a second wave of the virus in the process).
A vaccine scheme – ‘Arms Out to Help Out’, let’s call it – would instead offer each individual in Britain a sum of, say, £200 once vaccinated and a £50 referral bonus for successfully encouraging a friend to get vaccinated within an appropriate time-frame. This payment would instead reflect the ‘neighbourhood benefits’ for health. Scientists believe that vaccines will either reduce symptoms and possibly the duration of infection, making those immunised less likely to infect others, or, at best, confer immunity altogether – both of which protect others around you.
Paying people to be vaccinated is well grounded in economics. Social interactions today create ‘negative externalities’ – they risk transmitting a dangerous virus to others without compensating those affected. If we only judged the risks to ourselves of social activity, we would get too much risky behaviour collectively, and those people who did not want to get the disease, especially the elderly and those with pre-existing conditions, would bear too many of the costs – at best, having to stay locked at home, and at worst, getting ill and dying. Hence why governments compel us with extremely costly social distancing regulations.
The flipside to this is that partial or full immunity provides a positive externality. The more people that have immunity, the lower the risk to others of getting infected. What’s more, a vaccine that has passed clinical trials achieves these benefits without the costs associated with the ‘other’ route to herd immunity – letting the virus pass through the population, with more death and long-term complications associated with the disease.
When people are observing strict and costly distancing, the effective level of herd immunity may be low. But scientists still believe that herd immunity robust to us returning to normal behaviour may require up to 60% or more of the population to be immune.
Given any vaccine is unlikely to be 100% effective, high compliance levels are therefore necessary to ensure this threshold is met. A 70% effective vaccine, for example, would require around 85% of people to get the shot to pass this threshold. Yet a Kings College London-Ipsos-Mori poll in mid-August found that 16% of people already say they would be unlikely to or definitely wouldn’t be vaccinated; while another 20% were only ‘fairly likely’ to. Incentivising waverers may be the difference between achieving a herd immunity that allows normality or not.
The logic of externalities is why important vaccines are already subsidised through the NHS. But, in this case, the huge economic benefits of greater immunity, allowing these devastating social and business restrictions to be removed, suggest going further. A time-limited cash payment could really grease the wheels by providing a strong incentive to get vaccinated as soon as feasible.
It wouldn’t be cheap, of course. Paying £200 per vaccination (plus a £50 referral fee) would cost an additional £17 billion. But since the pandemic is currently costing us £20 billion a month in lost output – even before the eye-watering borrowing required to keep businesses and their staff afloat – the scheme would be cost-effective if it helped us reach herd immunity just one month earlier.
Might payments put people off by arousing suspicion about why the payments are necessary? The Government could begin surveying the country to gauge people’s receptiveness, although it’s difficult to believe the scheme would result in as much resistance as a coercive mandate that compelled people to be immunised by law.
And the evidence elsewhere suggests that money talks. Randomised control trials in Australia show that small financial incentives increased hepatitis B vaccination rates among drug users. A trial that gave vouchers worth £45 to girls in England increased take-up of HPV vaccinations by 50% compared to a control group. A study of American colleges found that students given a $30 incentive were more than twice as likely to get a flu vaccination as a control group. Nobel Prize-winning economists Abhijit Banerjee and Esther Duflo found that in India incentives for successful immunisation more than doubled take-up rates for children.
These extraordinary times have led to previously unthinkable policies. When a safe vaccine is feasible, we want to reap the economic benefits as soon as possible. Encouraging a rapid take-up via a payment and referral scheme could be the biggest economic stimulus available, harnessing private citizens to do the hard marketing themselves. When the time is right, the Chancellor should ready a final cash bazooka to end this pandemic once and for all.
Click here to subscribe to our daily briefing – the best pieces from CapX and across the web.
CapX depends on the generosity of its readers. If you value what we do, please consider making a donation.